Janapadodhvansa

Janapadodhvansa (also spelled as janapadodhvamsa) means destruction of communities due to a common cause. The affliction of diseases in society disrupting the physical, psychological, social health of community is phenomenon observed since inception of life on the earth. The pandemic and epidemic situations are considered to be as old as human evolution. Ayurveda texts have thus also extensively mentioned the pandemic conditions at various places commonly referred to as janapadodhvansa, maraka or janamara. Acharya Charak has explained the concept of janapadodhvansa in vimana sthana of the treatise Charak samhita. The concept of janapadodhvansais thus reference point for the description of disease origin and spread in the population highlighting the principles of epidemiology in ayurveda.
| Section/Chapter/topic | Concepts/Janapadodhvansa |
|---|---|
| Authors |
Bhojani M. K. 1, Joglekar Aishwarya 2 |
| Reviewer | Basisht G.3, |
| Editor | Deole Y.S.4 |
| Affiliations |
1 Department of Sharir Kriya, All India Institute of Ayurveda, New Delhi, India 2 Department of Department of Samhita Siddhant, All India Institute of Ayurveda, New Delhi, India 3 Rheumatologist, Orlando, Florida, U.S.A. 4 Department of Kayachikitsa, G. J. Patel Institute of Ayurvedic Studies and Research, New Vallabh Vidyanagar, Gujarat, India |
| Correspondence emails |
meera.samhita@aiia.gov.in, carakasamhita@gmail.com |
| Publisher | Charak Samhita Research, Training and Development Centre, I.T.R.A., Jamnagar, India |
| Date of publication: | May 16, 2023 |
| DOI | 10.47468/CSNE.2023.e01.s09.137 |
What is janapadodhvansa?
Janapadodhvansa is defined as a phenomenon in which a large population is inflicted with one particular disease irrespective of their prakriti (phenotype), ahara (dietary habits), dehabala (innate immunity and strength), satmya (behavioural habits and lifestyle) and sattva (mental conditions), vayasa (age group) (Cha.Sa. Vimana Sthana 3/6)
Etymology
Janapad refers to group of people/inhabitants or community while uddhwansa refers to the destruction of the community. Thus it is a condition where large group of people or entire community is destroyeddue to the natural or artificial phenomena.
Synonyms of janapadodhvansa
Janapadodhvansa is quoted as janamara by Acharya Bhela and Maraka by Acharya Sushrut (Su. Sa. Sutra Sthana 6/19) indicating the prevalence of epidemics in those times as well.
Causes of janapadodhvansa
Two types of causes of origin of diseases (vyadhi-utpatti hetu) are described. Common aetiological factors (sadharana hetu) can produce diseases in almost all the beings (bahujana sadharana).Specific etiological factors (asadharana hetu) are personalized and differ from individual to individual. (Chakrapani on Cha. Sa. Vimana Sthana 3/3)Janapadodhvansa chapter deals with the common causes of disease occurrence in large community.
The four main environmental factors like vata (vitiated air or atmospheric factors), jala (vitiated water), desha (geographical factors or those related to vitiated land and soil resources), kaala (seasonal and climatic conditions) are focused to cause epidemic situations. (Cha. Sa Vimana Sthana 3/6). These can be summarized as given in the table below: (Table No. 1 – Entity causative of janapadodhvansa and its interpretation in present context)
| Entity | Signs of vitiation | Present context |
|---|---|---|
| Vayu | Vishama vayu - showing characteristics contradictory to normal air conditions | This represents the climate change that causes impact on the social and environmental determinants of health.[1] |
| Atichala – fast blowing winds / squall | These are natural phenomena that can cause a loss of human and environmental resources over a large area.[2] | |
| Ati- stimita –stagnation of air | Poor air circulation and damp atmosphere promotes the spread of bacteria and viruses.[3] | |
| Atiparusha – excessive dryness | This can be correlated with low air humidity resulting in excessive dryness in air especially indoor air.[4] | |
| Ati sheeta- excessive cold air | Exposure to cold weather which can occur in the high altitude regions and extremes of climate especially during winter season.[5] | |
| Ati abhishyandi – overt humidity in air | An increase in air humidity that triggers rise in the occurrence of diseases.[6] | |
| Ati ushna- excessive heat in surrounding air | Excessive hot atmosphere can lead to conditions like heat exhaustion.[7] | |
| Ati kundalinaam- hurricanes or cyclones. | Cycloneis a system of storms or winds that rotate at centre of atmosphere with at a very high speed usually associated with heavy rains.[8] It possesses potential to destruct habitations over a large area. | |
| Asatmya gandha – foul smelling | Odor pollution is emerging risk factor for the populations exposed to industrial pollution, generalized climate change and environmental pollution.[9] | |
| Containing bashpa (fog), sikta (air pollutant like industrial effluents, solid pollutant particulate matter), panshu (micro pollutants), dhuma (smoke or smog) | The particulate matter is mixture of microscopic solids and liquid droplets suspended in air. These include pollutants like acids, organic chemicals, soil, dust particles and allergens.[10] | |
| Udaka (water) |
Vikruta gandha - altered odour Vikruta varna - altered colour Vikruta rasa - altered taste Vikruta sparsha, kleda bahula – altered consistency. |
These are the indicators of water pollution. All these conditions depict lack of acceptability of drinking water due to the presence of taste and odour which is otherwise absent in water suitable for consumption.[11] |
| Upakranta jalachara – Devoid of biota and animals due to the death of animals | This condition is similar to famine where the lands are devoid of biota as a cause of extreme scarcity of food and water resources.[12] | |
| Upaksheena jalashaya – drying up of water resources- indication of drought | Drought is a prolonged dry period in the natural climate cycle. This slow-onset disaster is characterized by lack of precipitation, resulting in a water shortage.[13] | |
| Apreetikara aapada guna –Water sources having questionable palatability and quality. | The water quality is affected by pollutants and particulate matter rendering it undesirable taste, odour, colour and consistency. If the drinking water is not of optimum quality, it threatens the overall health of community.[14] | |
| Desha (Soil or region) |
Dhoomrapavana – region having polluted atmosphere. Kshubhita salilashaya – pollution of available water resources. |
This can be compared with environmental pollution, overcrowding, altered quality of soil and water, lack of sanitation and resources.[15] |
| Vikruta varna – alteration in normal colour Vikruta gandha – altered smell, presence of odour otherwise absent in the drinking water vikruta sparsha – altered texture or consistency of water Kledabahula – excessive water content in the atmosphere or presence of stickiness |
This indicates the soil pollution. It is defined as the presence of toxic chemicals in the form of pollutants or contaminants in soil, in concentrations high enough to cause a risk to human health and/or the ecosystem.[16] | |
| Upasrushta sari srupa vyala mashaka makshika mushaka – having more organisms like flies, snakes, rats etc. Pratanadi bahula – excess growth of climbers and hyacinth especially in the water resources Atishushka nashta shasya – withering of crops Vyathita vividha mruga pakshi - Disturbed ecosystems |
This refers to the disruption of biota and ecosystems and environmental pollution leading to death of plants and animals in the region.[17] | |
| Nashta dharma aachara sheela – loss of sense of humanity and responsibility amongst the civilians | Disruption of social conduct and behaviour. These factors determine the effect on the social, behavioural determinants of health.[18] | |
| Pratata ulka pata - area more prone to occurrence of natural calamities like meteors etc. Bhumikampa – occurrence of earthquakes. |
This refers to susceptibility of region for the occurrence of natural calamities.[19] These are a sudden events in nature that usually results in serious morbidity and mortality. floods ,earthquakes, tornados etc. | |
| Kaala | Yatha ritu -viparita lakshana – excessive seasonal variations. yatha ritu- hina linga, ati linga |
Kaala factor is the seasonal occurrence of diseases. These also indicate the disease conditions arising from the disrupted climate.[20] |
Acharya Sushruta states vyapanna ritu (unfavourable seasons) as the primary cause of janapadodhvansa or maraca. Seasonal variations whether gradual or transient lead to disturbance in equilibrium of doshas, thus affecting the health of population. (Su. Sa. Sutra Sthana 6/21)
Adharma (inappropriate bahaviour) as a cause
Adharma (inappropriate behaviour) is another cause of janapadodhvansa can be described as not abiding to one’s prescribed duties and responsibilities. (Cha. Sa. Vimana Sthana 3/24) This can be associated with the human conduct and behaviour responsible for the occurrence of diseases. This reflects on the social determinants of health. The researches have proved that human behaviour is equally responsible in occurrence of epidemics as it results in excessive exploitation of natural resources, increase in pollution, increase in incidence of warfare, decreased social harmony, disturbance of ecosystems and deterioration of universal health.[21] Pragyaparadha (intellectual errors), shashtraprabhava (warfare), rakshogana (infectious conditions) and abhishapa (inappropriate social behaviour) are social, behavioral determinants of health. These can be termed as host specific factors for disease occurrence.
Adharma as a hetu of janapadodhvansa can be illustrated in the table as given below (Table No. 2 - Hetu of janapadodhvansa in purview of adharma)
| Hetu of janapadodhvansa in purview of adharma | |
|---|---|
| Prajnaparadha | Prajnaparadha is intellectual mistake or knowingly performing sinful or inappropriate actions. (Cha. Sa. Shareera Sthana 1/102) This can be compared with the imbalance in public health and lack of healthcare management systems, lack of personal hygiene and lack of awareness regarding preservation of health which affects the health of community.[22] |
| Shashtraprabhava | Casualties occurring due to the conditions like war, riots etc. It is the leading cause of deterioration of physical and mental health of many countries.[23] |
| Rakshogana | This represent the microbes that cause the disease.
Most common types of epidemics are of infectious type and have zoonotic spread. For example Spanish flu, Swine flu, Bird flu, Typhoid fever, Severe acute respiratory syndrome (SARS) and COVID-19 that have emerged in the recent times.[24] |
| Abhishapa | These refer to the compromised social and community manners and etiquette guidelines thus decreasing public health i.e. absence of sadvritta palana (code of conduct).[25] |
Thus the three major etiological causes of Janapadodhwans can be featured in the figure as given below- (Figure No. 1 – Major Hetu of Janapadodhvansa)

Jwara (fever) as a prime linga (~representative symptom) of janapadodhvansajanya vyadhi
Jwara is characterized as a condition affecting both physical and mental wellbeing. It is the chief disorder amongst all other diseases affecting every living being at the time of birth and death. (Cha. Sa. Nidana Sthana 1/35) Most of the epidemics related to infectious diseases are types of influenza or are almost always associated with fever.[26] Outbreak of Spanish Flu, dengue fever, swine flu, bird flu, typhoid, cholera, and even the present day COVID-19 are examples of jwara that resulted in some or the other form of janapadodhvansa.[27]
Sushruta (Su. Sa. Sutra Sthana 6/21) on the other hand has also explained few other manifestations of maraka like kasa (cough, bronchitis, lower respiratory tract infections), shwasa (respiratory infections, pneumonia), vamathu (gastric disturbance, nausea), pratishyaya (rhinitis, coryza or upper respiratory tract infections), shiroruja (headache) besides jwara. These are also commonly observed infectious diseases posing havoc in the community.
Similarly, Sushruta mentions that the infection can also spread through surface contact with things like beddings, blankets, seating arrangement, vehicles, jewellery and accessories. (Su. Sa. Sutra Sthana 6/21)
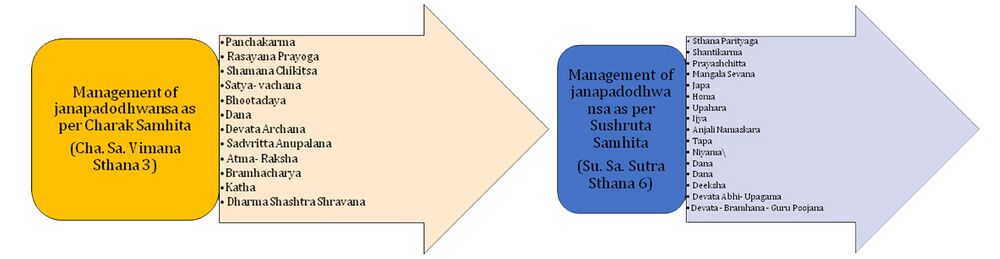
Management of janapadodhvansa
Acharya Charaka mentions the need of collection of medicinal herbs and commodities which are important for supporting the life in emergencies or epidemics beforehand, as there can be scarcity of the even most basic life needs during such period. [Cha. Sa. Vimana Sthana 3/4,13-18] This denotes the basis of disaster management and organization of healthcare facilities during epidemics. The hospitals should be well prepared with all the emergency and required facilities to combat the health consequences of disasters.[28]
The principal line of treatment in the management of diseases like jwara is pachana (medications enhancing digestion), vamana (therapeutic emesis) and apatarpana (depleting procedures). [Cha. Sa. Vimana Sthana 3/40] Ushnodaka (warm water) helps in achieving all the above criteria. It is also indicated for the treatment of jwara as it pacifies vata and kapha dosha. [Cha. Sa. Vimana Sthana 3/40] It facilitates digestion and relieves anorexia due to its deepana (appetizing), pachana (digestion) properties. It satiates thirst(trishna), when consumed even in small quantities. Its consumption is especially indicated in management of conditions like kasa (cough), peenasa (sinusitis), nava jwara (pyrexia), shwasa (breathing abnormality), etc. which represent majority of infectious diseases.[Cha. Sa. Chikitsa Sthana 22/58]
The generalized principles for management of janapadodhvansa include the measures for the promotion, preservation and correction of both physical and mental health. The panchakarma is the main line of treatment in these conditions. [Cha. Sa. Vimana Sthana 3/13] Vamana is important for the radical removal of vitiated dosha especially the kapha dosha and helps in pacifying the jwara and nausea (hrillasa) related conditions associated with the infection. [Cha. Sa. Chikitsa Sthana 3/146] Virechana also helps to evacuate the vitiated dosha through the faeces and corrects the agni vitiation. [Cha. Sa. Chikitsa Sthana 3/169) Basti controls the vitiated vata and helps in excretion of the toxins and fecal matter from the bowel region. [Cha. Sa. Siddhi Sthana 1/40] Due to nasya or nasal instillation invading pathogens get adsorbed on the surface restricting their growth and further progression. Nasya is thus particularly useful in the treatment and prevention of respiratory tract infections. Snehana (internal administration of ghee or oil) in form of go-ghrita (ghee). Jwara involves the obstruction of swedavaha strotas (body channels carrying sweat) hence it will help to expel the toxins by inducing the process of swedana. [Cha. Sa. Chikitsa Sthana 3/130] Deepana pachana treatments play an important role at every step in management as maintenance of agni function is of prime importance in prevention of any disease.
Dhoomapana is a treatment where the particulate matter in dhooma (medicated smoke) has anti-microbial activity and maintains integrity of respiratory tract. It is thus indicated in many respiratory conditions. [Cha. Sa. Sutra Sthana 5/27-32] Gandusha (Oil pulling), kavala (gargling), dantapavana (brushing or cleaning of teeth) act as mechanical barriers by avoiding the entry of pathogens through the buccal cavity. Sharira parimarjana (cleaning of body surface) and snana (bathing) measures contribute to cleansing of the body surfaces and also includes hasta, pada and mukha prakshalana i.e. hand and feet sanitization to prevent the spread of disease. [Cha. Sa. Sutra Sthana 5/93-94]
The rasayana chikitsa forms the backbone of treatment of janapadodhvansa as it is pivotal in enhancing the immune response to pathogenic external and internal invasion and stress. [Cha. Sa. Vimana Sthana 3/13] Different rasayana acting on pranavaha, rasavaha strotas, annavaha strotas depending on the dosha and site involvement can thus be implemented for management of janapadodhvansa vyadhi. Use of various rasayana like Chyavanaprasha rasayana [Cha. Sa. Chikitsa Sthana 1/1/62-74], Bramha rasayana [Cha. Sa. Chikitsa Sthana 1/1/41-57], Amalaki rasayana [Cha. Sa. Chikitsa Sthana 1/2/9-14] etc. are popular in clinical scenario for of maintenance of health during pandemic conditions.
Other non-pharmacological and psychotherapy based approaches like sadvritta palana (following proper code of conduct) and behavioural attributes like satyabhashana (honesty), bhootadaya (compassion), bali (sacrifice), devata archana (devotion), daana (charity), vriddhopaseva (showing care and empathy towards the elderly) are mentioned to facilitate the social and mental health. Providing support and care to people and families affected with pandemics is of vital importance to balance the psychological components of health especially during the pandemic like conditions. [Cha. Sa. Vimana Sthana 3/15-16]
Sadvritta emphasizes on the spread and containment of the sansargajanya vyadhi (infectious diseases) and their mode of transmission. [Cha. Sa. Sutra Sthana 8/18] The sadvritta focuses on various domains like physical health, social behaviour, psychological state, hygiene, food etiquettes thus providing holistic care.
The treatment and preventive aspects of epidemics in purview of ayurveda can be summarized in the following table-
| Other measures to ensure the promotion of health | |
|---|---|
| Promotion of mental and social health | |
| Behavioural attributes | |
| Practice of sadvritta |
|
| Shivanam upasevanaam (using means of protection) |
|
| Bramhacharya palana (Following safe sexual behaviour) |
|
| Dharma shashtranaam katha (Recreational measures) |
|
| Measures according to Sushruta Samhita | |
| Sthana Parityaga | |
| Shanti Karma |
|
| Prayaschitta |
|
| Japa (muttering a prayer/chanting repeatedly), homa (sacred offering to fire), Ijya (sacred offerings) |
|
| Anjali namaskara (greetings with folded hands, avoiding personal contact) |
|
| Tapa (following spiritual path), dana (charity), niyama (following proper regulations), daya (compassion), diksha (rites), guru abhigama (serving the elderly and teachers) |
|
Contemporary and applied aspects of janapadodhvansa
The concept of janapadodhvansa incorporates various aspects leading to causation of large number of diseases in large population or community. This further applies to the basics of public health or community health as mentioned in the Ayurveda texts. Thus striking similarities can be found in principles of epidemiology and concept of janapadodhvansa or maraka according to ayurveda. Some of these features are as mentioned below:
- Endemic nature of diseases: In janapadodhvansa chapter it is mentioned that Punarvasu Atreya assembled with his disciples including Agnivesha at banks of the river Ganga in Panchal Pradesh (present Northern India including regions of Uttar Pradesh). This is important to understand the region specificity or occurrence of the endemic diseases in the area. Endemic disease is the one which is predominantly present in the population in the given area e.g. chickenpox, malaria.[36] This concept can thus be correlated with medical topography which is the systematic surveying, mapping, charting, and description of specific geographical sites, with reference to the physical features that were presumed to influence health and disease.[37] Some diseases are more prevalent in northern hemisphere, some in southern, some occur more commonly in tropical region. For instance, Plasmodium falciparum is the type of vector of malaria that is geographically located in the tropical and subtropical areas and is the most common cause of disease.[38] Charaka Samhita also describes three types of topographical conditions by dividing the desha into jangala, anupa and sadharana. (Cha. Sa. Vimana Sthana 3/47-48). Jangala desha (dry land) has less biota, scarce water resources, more wind and sunlight while anupa (marshy land) has abundant biota and flora, stagnant or scarce winds and lacks sunlight. Climatic conditions in jangala desha are considered optimum for health and reduce the disease occurrence than those in anupa desha.
- Seasonal diseases: The discussion was held in the months of spring and summer seasons (gharma maasa i.e. in the jyestha and aashadha maasa vis a vis vasanta and greeshma ritu). This evidence suggests that there was a possibility of outbreak of some kind of communicable disease in that particular time and season in the described region. These seasons are homologous to spring and summer season which even in the present era witness the outbreak of various exanthemata’s, allergic conditions and different type of fever annually.[39]
- Epidemiological triad: Causative factors of janapadodhvansa can be compared to epidemiological triad which involves the external agent, susceptible host and environment. Interaction of these three components always leads to disease causation in large population and can be applied to both communicable and non-communicable diseases.[40] The concept of janapadodhvansa is similar to that of epidemic or pandemic, where epidemic is a condition affecting or tending to affect a disproportionately large number of individuals within a population, community, or region at the same time.[41] Pandemic is the condition occurring over a wide geographic area and affecting an exceptionally high proportion of the population.[42] According to epidemiology, the causative factors affecting the contraction of disease in population are similar to those mentioned in the chapter which includes geographic location (desha), climatic factors, biotic biological factors represented by plant related and zoological factors (vriksha (flora), mriga- pakshi (fauna)etc.) and abiotic or socioeconomic factors (janapada). The seasonality of diseases is important factor for the epidemicoutbursts throughout the globe.[43] The kala factor does play an important role in disease manifestation. Desha as mentioned earlier is important while considering the epidemiology, as outbreak of some diseases are region specific and their spread or progression also depends on the geographical, demographical and climatic conditions. It is helpful to understand the prevalence and incidence of diseases in the particular area.
The description of vitiated air (vishama or vikrita vayu) indicates climate change that increases the vulnerability of the populations to climate sensitive health risks like injury, mortality, temperature related illness (both hyperthermia and hypothermia), respiratory illnesses, zoonosis, vector borne diseases, malnutrition, communicable diseases, mental and psychosocial health etc.[44] Both atichala and atikundalinam vayu can be understood as fast blowing winds, cyclones, hurricanes or tornados that can result in public health emergencies like storm related mortality, injury, infectious diseases, impairment of mental wellbeing due to socio-economic factors like displacement, unemployment, disruption of ecosystems etc.[45] Atiparusha vayu or overly dry air indicates lack of humidity or excessive dryness in air contributing to the physical health related symptoms like dry eyes, itching of skin, dry throat etc. The stress on the nasal mucosa to humidify the entering air is intensified leading to be a major cause of respiratory disorders.[46] Atisheeta vayu or excessive cold air like that in air conditioned environments also poses a threat to increase in respiratory infections.[47] Epidemics like influenza have known to show a marked wintertime seasonality with over 2-3-month period within the months of November and March thus underlining the presence of cold air in atmosphere.[48] Atiabhishyandi or excessively humid air can intensify the heat and perspiration and trigger the respiratory conditions like asthma and COPD.[49] Ati-ushna vayu indicates the excessive rise in temperature which can cause heat stress related conditions like heat exhaustion and can also be a resultant of climate change and heat waves. It can also result in excessive dehydration.[50] Asatmya gandha indicates theodour pollution which is not only a determinant of environmental pollution but can also affect the physical health of community. It can result in occurrence of symptoms like wheezing, asthma, cough, headache, nausea and even mental stress related outcomes like mood changes.[51] The particulate matter or presence of pollutants in air is pressing problem due to advent of globalization and industrialization can also be correlated with asatmya gandha. Exposure to particulate matter can lead to reduced lung function, development of lung diseases like COPD, occupational lung diseases and even death.[52] Dushita Jala (impure water) also acts a carrier or cause of many epidemiological and endemic disorders. Most intestinal or enteric diseases are water borne infections. These are transmitted through faecal waste when the water is polluted by faecal matter.[53] Minamata Bay disease is excellent example of possible outbreak of severe disease through water pollution.[54] Many water borne bacterial infections can result in occurrence of disease like Typhoid(caused by Salmonella typhi), bacillary dysentery (caused by Shigella), viral infections like infectious hepatitis(Hepatitis A), Cholera(caused by Vibrio) and protozoal infections like amoebiasis, giardiasis etc. Upakranta and upaksheena Jalashaya indicate occurrence of famines and droughts. Droughts have far fetching consequences on the quality of public health resulting in the rise in infectious and nutrition related diseases. It results in shortage of drinking water and poor water quality and lack of hygiene.[55] Access to safe and quality drinking water is the prime necessity for livelihood. WHO has put forth guidelines and standards to rectify the quality of drinking water to safeguard the health of population. Waterborne diseases resulting from consumption of unhealthy drinking water poses a great threat to the high risk population like children, geriatric population, pregnant women and those suffering from debilitating diseases. The water quality can be affected by microbial content, presence of impurities like heavy metals, faecal matter and other solvents making it unsafe for consumption.[56] Desha dushti the third factor leading to causation of janapadodhvansa can be understood as soil pollution that results from exposure to soil with altered quality as there can be ingestion, inhalation or dermal absorption of the pollutants present in the soil.[57] This factor is also affected by over- crowding which leads to the lack of hygiene and sanitation increasing the risk of spread of infectious disorders. It can result in overburdening of healthcare facilities and lack of sustainable development, further intensifying the environmental pollution. Ecosystems have direct or indirect impact on health as they are major source of food, water, supplies and even livelihood for the population.[58] Disturbed ecosystems lead to the outbreak of various Zoonotic diseases. For instance, the overabundance of vectors like makshika (flies), mashaka (mosquitos) can relate to the spread of vector borne diseases like dengue and chikungunya. The natural disasters like ulka patina (meteors) and bhoomikapana (earthquakes) indicate the emphasis of Acharya on the physical, mental, social, economic burden caused by such mishaps on the millions of people increasing the incidence of morbidity and mortality due communicable diseases as well.
Kala factor is the most important amongst the aforesaid factors as it directly indicates the climate changes which is beyond intervention by human efforts. As mentioned earlier the spread and cause of infectious diseases follows a cyclic or calendar pattern and seasonal changes can lead to sudden rise of epidemic outbreaks.[59]
Recent researches
As mentioned earlier the pandemics have been a pressing problems since centuries altogether. The published data suggests that there have three pandemics of plague (since 5th century AD), 7 pandemics of cholera(17th century AD), Influenza related pandemics (17th century AD) like Russian Flu, Spanish Flu, Swine Flu, SARS (Severe Acute Respiratory Syndrome), MERS (Middle East Respiratory Syndrome) in the past and Covid 19 (21st century) being the most recent.[60] The data from WHO sugggets that Covid 19 is still prevalent in most of the parts of the world and as of 9 April 2023 more than 762 million confirmed cases and over 6.8 million deaths have been reported globally.[61]
The outbreak of COVID-19 pandemic attracted the attention of ayurveda fraternity towards the concept of Janapadodhvansa and its importance in preservation of health of entire community. Significant research work was thus carried out in this purview keeping janapadodhvansa in mind. Few such works are mentioned are mentioned belowHowever epidemiological assessment of various Hetu and Lakshana should be done accordingly
- In the review article entitled “Scientific aspects of Janapadodhvansa Vyadhi (epidemic disorders) according to Ayurveda in the context to Jwara—An epidemiological and Trisutra-based approach” authors have tried to throw light upon the scientific aspects of janapadodhvansa vyadhi in light of epidemiology by correlating the epidemiological triad with trisutra i.e. epidemiological triad i.e. Host, agent and environment.[62]
- Review article entitled “Conceptual study on Janapadodhvansa Roga and its treatment” focuses on the major causes of janapadodhvansa and purification of impure soil, water and air mentioned according to Ayurveda.[63]
- The review article, “janapadodhvansa in Ayurveda and its contemporary relevance to COVID-19” focuses on the implications of COVID-19, considering it as janapadodhvansajanya vyadhi and methods to curb to the same.[64]
- In the article , janapadodhvansaand its impact on Covid-19, authors have focused on the concepts relevant to janapadodhvansa in purview of aetiology, spread and management of novel disease COVID-19.[65]
- Authors have compared the different principles of janapadodhvansa to that of the epidemics in the review article entitled “Janapadodhwamsa : A Concept of Epidemic in Ayurveda”.[66]
- In the article entitled “Janapadodhwamsa - An Ayurvedic and modern overview in present era” the authors have tried to throw light upon the classical and contemporary approaches in understanding janapadodhvansa vyadhi.[67]
- In the article “Ayurveda considerations on Infectious diseases and their preventive measures w.s.r. to current pandemic situation” the janapdodhwansa vyadhi are compared with that of the infectious diseases which may lead to modern pandemics.[68]
- In the article entitled “Role of Rasayan In Communicable Disease (Janapadodhwamsa)” authors have thrown light upon the applicability of different rasyana in management of janapadodhvansa vis a vis communicable disease.[69]
- In the article “Review on preventive measures of Corona with special reference to janapadodhwamsa” authors have thrown light upon the various preventive measures for the management of janapadodhvansa vyadhi.[70]
- Considering the COVID 19 as a janapadodhvansa vyadhi, chemo-profiling and analytical assessment of different herbs in management of same is mentioned in the article ‘Chemical profiling of selected Ayurveda formulations recommended for COVID-19’.[71]
- In the article entitled “Ayurveda and Psychosocial impact of COVID-19”, authors have focused on the impact janapodhwansa janya vyadhi pose on the psychosocial health of individuals.[72]
Summary
The concept of janapadodhvansa is a testimony of the contribution of Ayurveda in the field of epidemiology and public health. The description of the major etiological factors like sadharana hetu (common spreading causes), adharma (not following code of conduct) and vyapanna ritu (unfavourable climatic conditions) shall be considerd while dealing with the epidemics or pandemics. Preservation of health through ayurveda measures like panchakarma (five purification therapies), rasayana (rejuvenation therapies), sadvritta (good code of conduct) are best measures for protection against pandemics. The treatments to promote good digestion and metabolism (deepana pachana) and disease specific therapies for jwara are important in case of occurance. Hygiene of external pathways like oral hygiene, nasal mucosal protection, bath, medicated smoking are measures to prevent microbial invasion and their growh in body. Thus the treatment of janapadodhvansa is a comprehensive protocol for personal and social health.
Related Chapters
Janapadodhvansaniya Vimana [Cha. Sa. Vimana Sthana 3], Ritucharya Adhyaya [Su. Sa. Sutrasthana 6]
Send us your suggestions and feedback on this page.
References
- ↑ Climate change [Internet]. [cited 2022 Jan 23]. Available from: https://www.who.int/westernpacific/health-topics/climate-change
- ↑ Eichelberger S, Mccaa J, Nijssen B, Wood A. Climate change effects on wind speed. NAm Wind. 2008 Jan 1;7:68–72.
- ↑ Bacteria and Viruses | American Lung Association [Internet]. [cited 2020 Apr 5]. Available from: https://www.lung.org/clean-air/at-home/indoor-air-pollutants/bacteria-and-viruses
- ↑ Choi SH, Lee SW, Hong YS, Kim SJ, Kim NH. Effects of atmospheric temperature and humidity on outbreak of diseases. Emerg Med Australas. 2007 Dec;19(6):501–8.
- ↑ Cold Related Illnesses | NIOSH |CDC [Internet]. 2020 [cited 2022 Jan 23]. Available from: https://www.cdc.gov/niosh/topics/coldstress/coldrelatedillnesses.html
- ↑ Wolkoff P. Indoor air humidity, air quality, and health – An overview. International Journal of Hygiene and Environmental Health. 2018 Apr 1;221(3):376–90.
- ↑ WHO | Information and public health advice: heat and health [Internet]. WHO. World Health Organization; [cited 2020 Apr 5]. Available from: http://www.who.int/globalchange/publications/heat-and-health/en/
- ↑ Definition of CYCLONE [Internet]. [cited 2022 Jan 21]. Available from: https://www.merriam-webster.com/dictionary/cyclone
- ↑ Ranveer A, Pawar P, Latake P. Odour Pollution and Its Measurement. International Journal for Research in Applied Science & Engineering Technology (IJRASET). 2015 Dec 1;3:221–9.
- ↑ Particulate Matter Effects on Health - Air (U.S. National Park Service) [Internet]. [cited 2022 Jan 19]. Available from: https://www.nps.gov/subjects/air/humanhealth-pm.html
- ↑ Water Quality Monitoring - A Practical Guide to the Design and Implementation of Freshwater Quality Studies and Monitoring Programmes, Edited by Jamie Bartram and Richard Balance, Published on behalf of United Nations Environment Programme and the World Health Organization, 1996, Page No.-1,2
- ↑ Famine Definition & Meaning - Merriam-Webster [Internet]. [cited 2022 Jan 23]. Available from: https://www.merriam-webster.com/dictionary/famine
- ↑ Drought [Internet]. [cited 2022 Jan 21]. Available from: https://www.who.int/westernpacific/health-topics/drought
- ↑ Common Perceptible Water Quality Issues [Internet]. [cited 2020 Apr 5]. Available from: https://www.wqa.org/learn-about-water/perceptible-issues
- ↑ Briggs D. Environmental pollution and the global burden of disease. Br Med Bull. 2003 Dec 1;68(1):1–24.
- ↑ What Is Soil Pollution | Environmental Pollution Centers [Internet]. [cited 2022 Jan 23]. Available from: https://www.environmentalpollutioncenters.org/soil/
- ↑ Corvalán C, Hales S, McMichael AJ, Millennium Ecosystem Assessment (Program), World Health Organization, editors. Ecosystems and human well-being: health synthesis. Geneva, Switzerland: World Health Organization; 2005. 53 p. (Millennium ecosystem assessment).
- ↑ Social determinants of health [Internet]. [cited 2021 Jul 21]. Available from: https://www.who.int/westernpacific/health-topics/social-determinants-of-health
- ↑ Definition of NATURAL DISASTER [Internet]. [cited 2022 Jan 23]. Available from: https://www.merriam-webster.com/dictionary/natural+disaster
- ↑ Grassly NC, Fraser C. Seasonal infectious disease epidemiology. Proc Biol Sci. 2006 Oct 7;273(1600):2541–50.
- ↑ Funk S, Salathé M, Jansen VAA. Modelling the influence of human behaviour on the spread of infectious diseases: a review. J R Soc Interface. 2010 Sep 6;7(50):1247–56.
- ↑ Organisation mondiale de la santé. Managing epidemics: key facts about major deadly diseases. 2018.
- ↑ Sidel VW, Levy BS. The health impact of war. Int J Inj Contr Saf Promot. 2008 Dec;15(4):189–95
- ↑ Piret J, Boivin G. Pandemics Throughout History. Front Microbiol. 2021 Jan 15;11:631736.
- ↑ Dempsey RC, McAlaney J, Bewick BM. A Critical Appraisal of the Social Norms Approach as an Interventional Strategy for Health-Related Behavior and Attitude Change. Frontiers in Psychology [Internet]. 2018 [cited 2022 Jan 23];9. Available from: https://www.frontiersin.org/article/10.3389/fpsyg.2018.02180
- ↑ Microbial Threats I of M (US) F on. Infectious Disease Emergence: Past, Present, and Future [Internet]. Microbial Evolution and Co-Adaptation: A Tribute to the Life and Scientific Legacies of Joshua Lederberg: Workshop Summary. National Academies Press (US); 2009 [cited 2020 Apr 4]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK45714/
- ↑ Baker RE, Mahmud AS, Miller IF, et al. Infectious disease in an era of global change. Nat Rev Microbiol. 2022;20(4):193-205. doi:10.1038/s41579-021-00639-z
- ↑ Hospital Preparedness for Epidemics [Internet]. [cited 2020 Apr 9]. Available from: https://www.who.int/publications-detail/hospital-preparedness-for-epidemics
- ↑ Umberson D, Montez JK. Social relationships and health: a flashpoint for health policy. J Health Soc Behav. 2010;51 Suppl(Suppl):S54-S66. doi:10.1177/0022146510383501
- ↑ Rational use of personal protective equipment for coronavirus disease (COVID-19) and considerations during severe shortages [Internet]. [cited 2020 Apr 10]. Available from: https://www.who.int/publications-detail/rational-use-of-personal-protective equipment-for-coronavirus-disease-(covid-19)-and-considerations-during-severe-shortages
- ↑ Sexually Transmitted Diseases - Information from CDC [Internet]. [cited 2022 Jan 23]. Available from: https://www.cdc.gov/std/default.html
- ↑ HIV/AIDS [Internet]. [cited 2022 Jan 23]. Available from: https://www.who.int/news-room/fact-sheets/detail/hiv-aids
- ↑ Hwang TJ, Rabheru K, Peisah C, Reichman W, Ikeda M. Loneliness and social isolation during the COVID-19 pandemic. Int Psychogeriatr. 2020;32(10):1217-1220. doi:10.1017/S1041610220000988
- ↑ Mental health (COVID-19) [Internet]. Public Health Sudbury & Districts. [cited 2020 Apr 10]. Available from: https://www.phsd.ca/health-topics-programs/diseases-infections/coronavirus/mental-health-covid-19
- ↑ Nair RR. Agnihotra Yajna: A Prototype of South Asian Traditional Medical Knowledge. Journal of Acupuncture and Meridian Studies [Internet]. 2017 Apr 1 [cited 2023 Apr 23];10(2):143–50. Available from: https://www.sciencedirect.com/science/article/pii/S2005290116301728
- ↑ Endemic Diseases-Types and Examples of Endemic Diseases [Internet]. BYJUS. [cited 2020 Apr 4]. Available from: https://byjus.com/biology/endemic-diseases/
- ↑ 4 questions with answers in MEDICAL TOPOGRAPHY | Science topic [Internet]. [cited 2020 Apr 4]. Available from: https://www.researchgate.net/topic/Medical-Topography
- ↑ Darshan Babu, Pampanna Gouda UTILITY OF THE KNOWLEDGE OF DESHA – A CLINICAL PERSPECTIVE; International Ayurvedic Medical Journal; Volume 3; Issue 3; March- 2015; ISSN:2320 5091
- ↑ Martinez ME. The calendar of epidemics: Seasonal cycles of infectious diseases. PLOS Pathogens. 2018 Nov 8;14(11):e1007327
- ↑ Principles of Epidemiology | Lesson 1 - Section 8 [Internet]. 2019 [cited 2020 Apr 9]. Available from: https://www.cdc.gov/csels/dsepd/ss1978/lesson1/section8.html
- ↑ Definition of EPIDEMIC [Internet]. [cited 2020 Apr 4]. Available from: https://www.merriam-webster.com/dictionary/epidemic
- ↑ Definition of PANDEMIC [Internet]. [cited 2020 Apr 4]. Available from: https://www.merriam-webster.com/dictionary/pandemic
- ↑ Components of the Triad | Models and Mechanisms of Public Health [Internet]. [cited 2020 Apr 4]. Available from: https://courses.lumenlearning.com/suny-buffalo-environmentalhealth/chapter/components-of-the-triad/
- ↑ Climate change and health [Internet]. [cited 2022 Jan 19]. Available from: https://www.who.int/news-room/fact-sheets/detail/climate-change-and-health
- ↑ James M. Shultz, Jill Russell, Zelde Espinel, Epidemiology of Tropical Cyclones: The Dynamics of Disaster, Disease, and Development, Epidemiologic Reviews, Volume 27, Issue 1, July 2005, Pages 21–35, https://doi.org/10.1093/epirev/mxi011
- ↑ Wolkoff P. Indoor air humidity, air quality, and health – An overview. International Journal of Hygiene and Environmental Health. 2018 Apr 1;221(3):376–90.
- ↑ Hyrkäs-Palmu H, Ikäheimo TM, Laatikainen T, Jousilahti P, Jaakkola MS, Jaakkola JJK. Cold weather increases respiratory symptoms and functional disability especially among patients with asthma and allergic rhinitis. Sci Rep [Internet]. 2018 Jul 4 [cited 2020 Apr 5];8. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6031646/
- ↑ Lowen AC, Steel J. Roles of Humidity and Temperature in Shaping Influenza Seasonality. J Virol. 2014 Jul;88(14):7692–5.
- ↑ Choi SH, Lee SW, Hong YS, Kim SJ, Kim NH. Effects of atmospheric temperature and humidity on outbreak of diseases. Emerg Med Australas. 2007 Dec;19(6):501–8.
- ↑ Kovats RS, Hajat S. Heat stress and public health: a critical review. Annu Rev Public Health. 2008;29:41–55.
- ↑ Tjalvin G, Magerøy N, Bråtveit M, Lygre Shl, Hollund Be, Moen Be. Odour as a determinant of persistent symptoms after a chemical explosion, a longitudinal study. Ind Health. 2017 Mar;55(2):127–37.
- ↑ Kelly FJ, Fussell JC. Air pollution and public health: emerging hazards and improved understanding of risk. Environ Geochem Health. 2015;37(4):631–49.
- ↑ Health impacts of water pollution [Internet]. [cited 2020 Apr 5]. Available from: http://edugreen.teri.res.in/explore/water/health.html
- ↑ Harada M. Minamata disease: methylmercury poisoning in Japan caused by environmental pollution. Crit Rev Toxicol. 1995;25(1):1–24.
- ↑ Health Implications of Drought | CDC [Internet]. 2020 [cited 2022 Jan 19]. Available from: https://www.cdc.gov/nceh/drought/implications.html
- ↑ World Health Organization. Guidelines for drinking-water quality: first addendum to the third edition, volume 1 : recommendations. Geneva: WHO; 2006.
- ↑ Landrigan PJ, Fuller R. Environmental pollution: An enormous and invisible burden on health systems in low- and middle-income counties. World Hosp Health Serv. 2014;50(4):35–40.
- ↑ Corvalán C, Hales S, McMichael AJ, Millennium Ecosystem Assessment (Program), World Health Organization, editors. Ecosystems and human well-being: health synthesis. Geneva, Switzerland: World Health Organization; 2005. 53 p. (Millennium ecosystem assessment)
- ↑ Martinez ME. The calendar of epidemics: Seasonal cycles of infectious diseases. PLOS Pathogens. 2018 Nov 8;14(11):e1007327.
- ↑ Piret J and Boivin G (2021) Pandemics Throughout History. Front. Microbiol. 11:631736. doi: 10.3389/fmicb.2020.631736
- ↑ Weekly epidemiological update on COVID-19 - 13 April 2023 [Internet]. [cited 2023 May 5]. Available from: https://www.who.int/publications/m/item/weekly-epidemiological-update-on-covid-19---13-april-2023
- ↑ Joglekar AA, Vyas MK, Bhojani MK. Scientific aspects of Janapadodhwansa Vyadhi (epidemic disorders) according to Ayurveda in the context to Jwara—An epidemiological and Trisutra-based approach. J Indian Sys Medicine [serial online] 2022 [cited 2023 Apr 23];10:176-85. Available from: https://www.joinsysmed.com/text.asp?2022/10/3/176/357681
- ↑ Anuradha G. Patil, Hemlata Krishnarao Belorkar, Conceptual study on Janapadodhvansa Roga and its treatment. J Ayu Int Med Sci. 2022;7(1):275-278. Available From- https://jaims.in/jaims/article/view/1702
- ↑ Wale Savita, Shingadagav Amol, Janapadodhwansa in Ayurveda and its Contemporary Relevance to COVID-19, Aayushi International Interdisciplinary Research Journal (AIIRJ), Vol- VII Issue- V May 2020, Page No. 56-60.
- ↑ Kabi C, Venate P, Prasad R. JANAPADODHWANSA AND ITS IMPACT ON COVID-19. e-Şarkiyat İlmi Araştırmaları Dergisi/Journal of Oriental Scientific Research (JOSR). 2021 Jul 1;XCI:93–105.
- ↑ Khayamali R, Khayamali B, Khayamali R. Janapadodhwamsa: A Concept of Epidemic in Ayurveda. Journal of Ayurveda Campus. 2022 Jun 24;2:46–53.
- ↑ Tarun Kumar Kushwaha, Suman Yadav, Ashutosh Kumar Yadav, Janapadodhwamsa - An Ayurvedic And Modern Overview In Present Era, Innovare journal of Ayurvedic Sciences Vol 9, Issue 6, 2021 , Page No. 1-5
- ↑ Naharia, R., and A. P. Verma. “Ayurveda Considerations on Infectious Diseases and Their Preventive Measures W.s.r. To Current Pandemic Situation”. Himalayan Journal of Health Sciences, Vol. 6, no. 2, June 2021, pp. 29-32, doi:10.22270/hjhs.v6i2.97.
- ↑ Shukla et. al. “Role of Rasayan in Communicable Disease (Janapadodhwamsa)” ejpmr, 2019,6(1), 232-234
- ↑ EBSCOhost | 152121539 | Review On Preventive Measures Of Corona With Special Reference To Janapadodhwamsa. [Internet]. [cited 2023 Apr 23]. Available from: https://web.p.ebscohost.com/abstract?direct=true&profile=ehost&scope=site&authtype=crawler&jrnl=09769242&AN=152121539&h=dAYAG8QLtmPPHjUk6VvIBcR03w4ehphQ9R5ccf4kaGBe4nu5xPHJZXWjh0SviVwi3bVOHL9Ejg%2fSsRnTut13FQ%3d%3d&crl=c&resultNs=AdminWebAuth&resultLocal=ErrCrlNotAuth&crlhashurl=login.aspx%3fdirect%3dtrue%26profile%3dehost%26scope%3dsite%26authtype%3dcrawler%26jrnl%3d09769242%26AN%3d152121539
- ↑ C. T., S., M., D., P. R., R. et al. Chemical profiling of selected Ayurveda formulations recommended for COVID-19. Beni-Suef Univ J Basic Appl Sci 10, 2 (2021). https://doi.org/10.1186/s43088-020-00089-1
- ↑ Mehta, Tanuja; Sharma, Uttam Kumar1; Mittal, Bhawana2. Ayurveda and Psychosocial Impact of COVID-19. Journal of Ayurveda 14(4):p 138-142, Oct–Dec 2020. | DOI: 10.4103/joa.joa_224_20