Acid peptic diseases
| Section/Chapter/topic | Concepts and Contemporary Practices -Nidana Chikitsa / Vyadhi / Acid peptic diseases |
|---|---|
| Author | Prof. Dr. H.M. Chandola1 |
| Reviewer | Basisht G.2 |
| Editors | Deole Y.S.2, Anagha.S.2, Basisht G. 2 |
| Affiliations |
1Former Dean I.P.G.T. & R.A, Jamnagar & Director-Principal, C.B.P.A.C.S., Delhi, India 2Charak Samhita Research, Training and Development Centre, I.T.& R.A., Jamnagar, Gujarat, India |
| Correspondence email: |
drharimohan.chandola@gmail.com, carakasamhita@gmail.com |
| Publisher | Charak Samhita Research, Training and Development Centre, I.T.R.A., Jamnagar, India |
| Date of first publication: | May 27, 2021 |
| DOI | 10.47468/CSNE.2021.e01.s09.057 |
Principles of diagnosis and management of acid peptic diseases in Ayurveda
This article is based on the lecture delivered by Prof. H.M. Chandola, as part of Prof. M.S. Baghel Memorial Lecture Series on 09th April 2021.The video lecture can be accessed on the link of facebook page.
Introduction
In the present era, the world is changing focus on “preservation of health” rather than treating the diseases. New diseases are emerging day by day in new forms. It is high time to recognize the importance of boosting up the defense mechanism of the body. This helps to resist any kind of adverse circumstances and maintain the proper balance of all the components of health.
Acharya Sushruta’s definition of a “healthy person” (swastha) is the most widely accepted one in Ayurveda.[Su. Sa. Sutra Sthana 15/41]
The physical components of health are listed as the three dosha - (vata, pitta and kapha); the seven body tissues (dhatu); and the excretory functions(mala). Digestive power (agni) is also added with due importance. It indicates that all kinds of “transformation processes”, essential for the maintenance of health are facilitated by the agni from gross to minute level.
Apart from physical health, the pleasant state and harmony of sensual faculties (indriya), mind (manas) as well as spiritual awareness (atma) are also the essential criteria for health. All these components are interrelated and can affect each other's state of well-being.
E.g: mental disturbances or negative emotions can disturb the proper function of digestive power and vice versa. If a person is worried, sad, angry, or emotionally upset, even the wholesome food consumed in proper quantity will not get digested properly.[Cha. Sa.Vimana Sthana 2/9]
Three categories of agni
Good health begins in the gut. While explaining the concept of agni, the main form of agni is called as the “jatharagni” (pachakagni) which refers to the digestive enzymes. There are five elemental enzymes (bhutagni) which are the micro-elemental converters, and also the seven corresponding tissue building enzymes (dhatwagni). The digestive enzymes (pachakagni) control the other two kinds of agni that are acting at the level of absorption and metabolism. The term “koshthagni” is used when it deals with the digestive process in the gastrointestinal tract (GIT).
Agni and patterns of digestion
When the agni is in the balanced state, it is known as “samagni”. But when it is affected by three dosha, it shows three pathological variations. If there is an excess of kapha dosha, it lowers the power of agni and the condition is known as “mandagni” (slow digestion). When pitta is in excess form, the agni becomes “teekshnagni” (fast/quick digestion). It can digest anything and everything and when the food is not available, it starts digesting the tissue elements (dhatu). For example, in thyrotoxicosis the hyperactivity of the thyroid gland causes high basic metabolic rate (BMR) and cachexia develops. When the agni is affected by vitiated vata, it becomes “vishamagni” (irregular digestion). As vata has catalytic action (“yogavahi”), if it interacts with kapha, it will enhance the activity of kapha and if it interacts with pitta, it enhances the activities of pitta.
Ultimately, the impairment of agni leads to improper digestion leading to the process of fermentation and putrefaction, and then, there is the production of toxic metabolites called "ama". These toxic metabolites are the main cause of all the disease conditions. All diseases arise from the lowered activity of agni.i.e “mandagni” [A.Hr. Chikitsa Sthana 12/1].
So, good or bad health begins in the gut and the treatment is focused on the measures for maintaining the health of digestive power (kayagni), thereby eliminating all the diseases of the whole body. This is the first branch of Ayurveda called “Kayachikitsa’.
The concept of digestion in Ayurveda
The whole digestive process in the gut starts right from the mouth, where there is the action of “bodhaka kapha” to start the process of digestion. Then it goes to the stomach (amashaya) where it is subjected to the action of "kledaka kapha" for adding the moisture content (kleda) to the food material. Subsequently, from the stomach (amashaya) it goes into the portion of the small intestine called "grahani" which is the seat of "pachaka pitta". The 6th internal layer called "pittadhara kala" is also situated there. The main process of digestion occurs in this portion of the gut. It is followed by caecum (unduka) and large intestine (pakwashaya) where the separation of essence (sara) and excretory materials (kitta) occurs with the help of “samana vayu” which leads to the absorption and assimilation of nutrient portion and excretion of the waste products in the form of faeces (purisha) and urine (mutra) with the help of “apana vayu”.
Here, the “kledaka kapha” can be represented in the form of mucin, which moistens the food materials and loosens its molecules. It buffers the action of the strong acid and inhibits the action of pepsin. It provides a protective layer to the stomach wall to prevent the corrosive effect and its digestion by pepsin. So, the functions of “kledaka kapha” are reflected mainly through the functions of mucin.
The action of kledaka kapha is also executed by the following secretions in the gut.
- Serous & mucous secretions of salivary glands & esophagus.
- Mucous secreted by mucous glands of surface mucous cells and mucous neck cells of the stomach.
- Mucous and bicarbonate ions secreted from bruner's gland of the small intestine.
- Bicarbonate ions secreted from the duct of pancreas.
- Alkaline mucous secretion by Brunner's glands in the duodenum.
- Mucous secreted by goblet cells that lubricate the intestinal surface.
- Water & electrolytes secreted by enterocytes of the small intestine.
- Mucous secreted by epithelial cells of crypt's of Liberkuhn of the large intestine.
“Pachaka pitta” represents the digestives enzymes like trypsin, chymotrypsin, carboxypolypeptidase, pancreatic amylase, pancreatic lipase, cholesterol esterase, phospholipase, salivary amylase, maltase, lingual lipase, pepsin, gastric lipase, gastric amylase, gelatinase, urase, etc.
It digests the food, separates the waste and nutrients from it, and supports the other forms of pitta located in different parts of the body.
The third most important component of the digestive process is “samana vayu” which represents the regulation of the enteric nervous system, the sympathetic and parasympathetic supply of the autonomic nervous system.
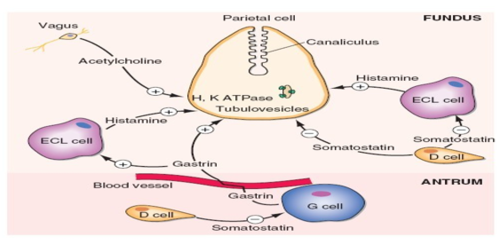
The action of "samana vayu" can be partially understood by the regulation of the secretion of HCL by parietal cells. The activities of the vagus nerve, the amount of gastrin from G cells and somatostatin from D cells, and the level of histamine play a vital role in this process.
Acid-Peptic Diseases
Acid peptic disorders include many conditions whose pathophysiology is directly related to the damage caused by acid and peptic activity of gastric secretions. It includes gastroesophageal reflux disease, peptic ulcer (gastric and duodenal), and stress-related mucosal injury. In all these conditions, mucosal erosions or ulcerations arise when the caustic effects of aggressive factors overwhelm the defensive factors of the gastrointestinal mucosa.
Aggressive and defensive Factors
Here, the aggressive factors represent the acid, pepsin, bile salts, drugs (NSAIDs), and H. pylori and the defensive factors are represented by mucus, bicarbonate layer, proper blood flow, cell renewal prostaglandins, and phospholipids.
So, the therapy is directed at enhancing host defence or eliminating aggressive factors including Helicobacter pylori. In short, the imbalance between aggressive factors (pachaka pitta) and defensive factors (kledaka kapha) leads to acid peptic diseases.
Vitiation of Agni (Agni dushti) and Acid peptic disorders
For maintaining health,agni should be in its balanced state, i.e. “samagni”. All other states of agni leads to acid peptic disorders. Improper dietary habits cause vitiation of agni, which leads to the process of fermentation of food material and ultimately it forms the toxic material called “amavisha”. It leads to “indigestion” (ajeerna) by vitiating the dosha. Continuous indulgence in improper diet and erratic lifestyle aggravates pitta dosha. This leads to an acute condition of “vidagdhajirna”. This is converted into different acid-peptic disorders like gastritis, gastro-oesophageal reflux disease(amlapitta), duodenal ulcer (parinama shula), gastric ulcer(annadrava shula) etc.
Vidagdhajeerna and Amlapitta
The clinical diagnosis of “vidagdhajeerna” is based on the symptoms like sour eructation, burning sensation, giddiness, thirst, and sweating. In case of “amlapitta”, the symptoms are indigestion, nausea, sour/bitter eructation, burning sensation in oesophagus, epigastric region, anorexia, and abdominal heaviness. Many of the clinical researches on “amlapitta” had revealed that hyperacidity might not be an essential finding in all the patients with the symptoms of “amlapitta”. Many of them can be normosecretors. Some may be hyper secretors as in the case of “hyperchlorhydria” and some may even be hypo-secretors as in the case of hypochlorhydria. For proper digestion, an appropriate pH is essential which is usually acidic in the stomach. A delayed gastric emptying time leads to fermentation of food, producing organic acids as seen in conditions like gastroparesis (alasaka - vilambika), whereas rapid gastric emptying acidifies the medium of gut. These states are seen in “amlapitta” and related diseases. Here, mucosal resistance is very important. The abnormal acid medium erodes the mucous lining of the concerned segment of the gut leading to painful conditions of the upper abdomen like gastric ulcer (annadrava shula) and duodenal ulcer (parinama shula). So, where aggressive factors are dominant, like in hyper-secretors, it leads to duodenal ulcer (parinama shula). Where there is the weakness of defensive factors, like in hypo-secretors or normo-secretors, it leads to the gastric ulcer (annadrava shula). So, it is better to consider amlapitta as a syndrome (acid reflux syndrome) rather than a particular gastrointestinal disease. It closely resembles gastritis, non-ulcer dyspepsia, hyperchlorhydria as well as hypochlorhydria and in the chronic stage, it may lead to gastric ulcer.
Gastritis
Gastritis is a clinical condition with upper abdominal discomfort like indigestion or dyspepsia in which specific clinical signs or radiological abnormalities are absent. It is of two types- acute gastritis and chronic gastritis.
Acute gastritis
For acute gastritis, there are many causative factors including diet and personal habits like consumption of highly spiced food, excessive alcohol consumption, heavy smoking, infections like H. Pylori, viral hepatitis, drugs like NSAIDs, aspirin, chemotherapeutic agents, severe stress including emotional factors like anger, shock, resentment, trauma, surgery and excessive burn. Due to these stress factors and smoking habits, the tracheobronchial tree of the person becomes hypersensitive and there will be increased secretion of acetylcholine, catecholamines, and histamine. This leads to hypersecretion of HCL from parietal cells due to hyperstimulation of vagus and increased secretion of gastrin. It makes the person more prone to acid peptic disorders.
It is better to take advantage of recent technologies for finding out the exact cause of the condition. If the conventional Ayurvedic treatment is not giving the desired result, we should explore the other possibilities like H.pylori infection and treat accordingly.
Principles of treatment in acute gastritis
- The related organ, stomach (amashaya) should be given due importance. ( amashaya vishesha chikitsa)
- Drugs that reduce the penetrating power (tikshnatva) and fluidity (dravatva) of pitta i.e, drugs having a bitter taste (tikta rasa) and dry (ruksha) nature should be used to counteract these properties respectively.
- Improving the quality of digestive power (agni deepana)
- Mild purgation (mridu virechana)
- Medicated enema containing milk (kshira basti)
- The formulations like Guduchyadi Kashayam, Patoladi Kashayam, Avipattikara churna, combination of Narikela lavana and Yashti churna are effective medicines in this condition.
- It is better to avoid fermented preparations (asava & arishta)
Chronic gastritis
Recurrent attacks of acute gastritis may result in chronic gastritis.
It is classified into,
- Type A gastritis (Autoimmune gastritis)
- Type B gastritis (H. Pylori related)
- Type AB gastritis (Mixed gastritis, environmental gastritis, chronic atrophic gastritis)
Type A gastritis – Auto immune gastritis
It mainly involves the body-fundic mucosa and is called autoimmune gastritis and is usually associated with other autoimmune diseases such as Hashimoto’s thyroiditis and Addison's disease. Antibodies against parietal cells and intrinsic factor cause depletion of parietal cells and this leads to the impaired secretion of intrinsic factors. Ultimately, these changes may lead to significant gastric atrophy.
Type B gastritis (H. Pylori infection)
It mainly involves the region of antral mucosa and is the common type. It is also called hypersecretory gastritis because of excessive secretion of acid due to H. Pylori infection. It is usually associated with peptic ulcer.
Type A B gastritis (Mixed / Environmental / Chronic atrophic gastritis)
It affects the mucosal region of the body of the stomach-both fundic and antral parts. It is the most common type of gastritis affecting all age groups. It is also called environmental gastritis because a number of unidentified environmental factors have been implicated in etiopathogenesis.
In its advanced stage, there is progression from chronic superficial gastritis to chronic atrophic gastritis characterized by mucosal atrophy and metaplasia of intestinal or pseudopyrloric type.
Principle of treatment of chronic gastritis
For treating the chronic gastritis, the principle of treatment of “vata-pitta dominant gulma” is recommended. It includes protecting the kapha, which is the defensive factor. Here, the measures to reduce the penetrating power (tikshnatva) of pitta should be administered, followed by healing or soothing type of medicines (ropana chikitsa). The combination of Glycyrrhiza Glabra (yashtimadhu), Asparagus racemosus (shatavari), Phyllanthus emblica (amalaki) with ghee and honey is best for healing action. Drugs with bitter (tikta) or sweet (madhura) tastes (rasa) are preferable here. Ghee or milk preparation processed with these kind of drugs are also advisable.
The psychological component should also be addressed with equal importance because stress plays an important role in this condition. If a person’s mental status is not positive, it may lead to indigestion.
In the second line of treatment, mild purgation therapy (mrudu virechana) can be given. It is better to avoid the ready-made decoctions (kashayas) in bottles because the preservatives added to them can worsen the condition. Medicated ghee preparations are better to be prescribed.
Formulations like avipattikara churna, sitopaladi churna, yashtitriphala churna, dadimadi ghrita, shatavari ghrita, guduchyadi ghrita, ashwagandha mahatiktam ghritam are effective in this condition.
Gastro-esophageal reflux disease (GERD)
Due to decreased tone of lower oesophageal sphincter, the gastric contents get regurgitated frequently into the oesophagus. It causes damage to the mucous membrane of oesophagus and lead to esophagitis.The risk factors for this condition include obesity, fat-rich diet, caffeine, alcohol, smoking, and the symptoms are heartburn, regurgitation, and dysphagia. It can be diagnosed on the basis of clinical symptoms, 24 hour pH monitoring, endoscopy, and biopsy.
Line of treatment of GERD:
“Amlapitta chikitsa” and “pittaja udavarta chikitsa” are recommended here. “Ama pachana” and “Vata anulomana” are the principles to be followed.
As vitiated vata is responsible for the opposite (upward) movement of gastric contents, measures to pacify vata and establish its natural downward movement (vatanulomana) is to be administered. Drugs that alleviate pitta and kapha, that dries up the moisture content (kledahara), and have a bitter taste (tikta rasa) predominantly are used here.
As the second line of treatment, drugs having a sweet taste (madhura rasa) are also prescribed.
In this condition, mild therapeutic emesis (sadyo vamana), mild therapeutic purgation (mrudu virechana), medicated enema containing milk (kshira basti) are also recommended. It is better to avoid fermented preparations (asava & arishta).
Avipattikara churna, vaishvanara churna, yashtimadhu churna are effective in this condition. After curing symptoms, ghee-based preparations (ghrita kalpana) like dadimadi ghrita , mahatiktaka ghrita, etc. should be prescribed for avoiding recurrence.
In the last phase, drakshadi lehya, dashamula haritaki avaleha, kushmanda rasayana, kalyana gud and shatavati gud are advisable.
Pravala bhasma, shankha bhasma and narikela lavana, act as good antacids. Kamadudha rasa, pravala panchmruta rasa, sutashekhara rasa are very effectively used in this condition.
The main thing is the modification of dietary and personal habits. It is better to avoid hot and spicy foods, excessive use of pungent, sour, and salty food, fried items, curd, mustard, and sour fruits in the diet. It is recommended to avoid alcohol consumption, smoking, and regular intake of coffee.
Peptic ulcer
It includes both gastric ulcer and duodenal ulcer formed due to the imbalance of aggressive factor and defensive factor as discussed earlier. Eating worsens the symptoms of gastric ulcer and improves the symptoms of duodenal ulcer. Hunger pain is observed in duodenal ulcer. The diagnosis is based on endoscopy. For detection of H. pylori, “rapid urease test” or “clo test” is performed. Biopsy is done to exclude possibility of cancer. In the management, high dose of proton pump inhibitors is given in conventional medicine.
Gastric ulcer (annadrava shula)
In this condition, there is continuous severe pain not subsiding in any stages of digestion like after digestion or during digestion, whether at empty stomach or after taking food. It is relieved only after vomiting out the accumulated pitta. [M. Ni. Shula Nidana]
Duodenal Ulcer (Parinama shula)
Vata vitiated due to its causative factors, gets mixed and blocked by morbid pitta and kapha. It causes severe pain (shula), which is known as “parinama shula”.
Excess pitta or acidic secretions damage the mucous layers (kapha) of the duodenum. The mucous layer sheds from its place and gets admixed with pitta (acids). Since the mucous layer forms a buffer and protective sheath of the intestines, shedding of the mucous membrane (kapha) leads to the formation of ulcers or sores in the intestinal mucosal walls. This is the stage of ulcer formation.
The vayu gets aggravated and causes severe pain. This may be correlated with the irritation of nerve fibers at the region of sores. When the acidic food from the stomach enters the duodenum for further digestion, it corrodes and irritates the sores causing severe pain during the process of digestion. The pain remains until the acidic food is pushed forward from the duodenum or until the afflicted person consumes food.
In vata predominant type of duodenal ulcer, abdominal distension, gurgling sound, and non-passage of stool and urine are the main symptoms. It is relieved by the use of unctuous and hot substances.
In pitta predominant type, there is excessive thirst, burning sensation, restlessness, and sweating. It is aggravated by the use of a spicy, sour, and salty diet. The pain is relieved by the use of cold articles.
In kapha predominant type, vomiting, nausea, disorientation are the main symptoms. Mild pain persists for a long time and relieved by pungent and bitter foods.
In case of peptic ulcer, rice, bean, salt, sour food articles, and condiments should be avoided. Milk, banana, and coconut water are advisable.
Principles of treatment of peptic ulcer
As the first line of treatment, drugs having predominantly bitter taste (tikta rasa) and inducing dryness(ruksha) are used.
In the second phase, drugs with sweet taste (madhura rasa) and bitter taste(tikta rasa), and medicated milk preparations are used.
In the last phase, medicated milk processed with drugs having sweet and bitter tastes is preferred. It is added with mental-health promoting (medhya) drugs. Avoiding the causative factor is the most important step in treatment. Mild purgation, enema with medicated milk (kshira basti), pouring of medicated buttermilk on the forehead (takradhara), and anointment of medicated paste on forehead or scalp (shirolepa) are effective procedures in this condition.
In a research work on duodenal ulcer(parinama shula) by Antony Jose & H.M.Chandola(2004), a formulation called “Akshadi churna” [a combination of Terminalia chebula (haritaki) , Terminalia bellirica(bibhitaki) , Phyllanthus emblica (amalaki) and Piper longum(pippali)][ Chakradatta 27/6] along with ghee preparation called “medhya rasayana ghrita”[a combination of Convolvulus pluricaulis(shankhapushpi) , Centella asiatica(mandukaparni), Glycyrrhiza Glabra (yashtimadhu) and Tinospora cordifolia (guduchi) ] were used. It showed better results than administering only Akshadi churna. Significant difference was observed in the parameters of Brief Psychiatry Rating Scale. This shows the importance of dealing with the psychic component in this disease.
Inflammatory bowel Diseases (IBD)
This includes two idiopathic bowel diseases having many similarities but distinctive morphological appearance.
a) Crohn’s disease (regional enteritis)
It affects the segment of terminal ileum and/ or colon, though any part of the gut may get involved.
b) Ulcerative colitis
It is the acute and chronic ulcero-inflammatory colitis affecting chiefly the mucosa and submucosa of the rectum and descending colon. Sometimes it may involve the entire length of the large bowel.
The etiological factors of IBD include genetic factors, immunologic factors, microbial factors, and environmental factors like long-term administration of NSAIDs, psychological factors, smoking, oral contraceptive pills etc. In a genetically predisposed individual, the effect of environmental factors and deranged microbiota, result in dysregulation of mucosal and immune function, which leads to chronic inflammation. It is diagnosed using endoscopy with tissue biopsy, colonoscopy, flexible sigmoidoscopy etc.
Symptoms like the elimination of faecal matter mixed with blood and mucous, having offensive smell are observed with weight loss in patients.These conditions are mentioned in the contexts of raktatisara, tridoshaja atisara and shokaja atisara. These symptoms are similar to IBD.
Principle of treatment for ulcerative colitis
The treatment protocols of “pittatisara” or “raktatisara”, “pitta-kapha grahani chikitsa”, “jirna pravahika chikitsa”, “adhoga raktapitta chikitsa” are adopted here. Anti-inflammatory (pakahara and shophahara) and anthelminthic (krimighna) treatments are preferred in cases of ulcerative colitis. Drugs having bitter (tikta) or sweet (madhura) taste, with healing (ropana) property, in the form of medicated milk are recommended here.
In the chronic stage, and if there is excessive blood loss, weight loss, the treatment for anaemia (pandu) and emaciation (dhatukshaya) also should be done.
The decoction preparations like drakshadi kashaya, ambashthadi gana kashaya, mahatikta kashaya, jivaniya gana kshira kashaya, guduchyadi kashaya, musta kshira kashaya etc. and the fermented preparations like lodhrasava, jirakarishta, kutajarishta, madhukasava, mustakarishta etc. are effective in this condition. However, fermented preparations should not be prescribed in the bleeding phase.
Medicines in the powder (churna) form namely dadimashtaka churna, kapitthashtakam churna, laksha churna with honey, lodhra-yashti churna, and pushyanuga churna are effective. Tablets like jatiphaladi gutika and bilvadi gutika are also prescribed.
Medicated ghee preparations like changeryadi ghrita, mahatiktaka ghrita and shatavari ghrita are effective. Buttermilk is a very good remedy to treat this condition. The formulation panchamrita parpati along with butter milk gives excellent relief when administered orally or per rectal route. The other preparations like swarna parpati, rasa parpati, bola parpati, dhatri loha, sutashekhara rasa, punarnava mandura etc. are also used for the treatment of ulcerative colitis.
Medicated milk preparations using Holarrhena antidysenterica(kutaja), Aconitum Heterophyllum(ativisha), Salmalia malabarica (shalmali), Vetiveria zizanioides (ushira), Symplocos racemosa roxb(lodhra), Woodfordia fruticosa(dhataki), and Nymphaea caerulea(utpala)are prescribed. Goat’s milk (aja kshira) is especially preferred for consumption.
The medicated enema called “pichcha basti” is observed as very effective in this condition.
Irritable Bowel Syndrome (IBS)
IBS is a psychosomatic intestinal motility disorder presenting as altered bowel habits, abdominal pain, and the absence of detectable organic pathology. Altered bowel habits, i.e. frequent constipation and diarrhea or any one of these two symptoms is observed as the main characteristic feature.
In Ayurvedic parlance, it can be interpreted under the following clinical conditions.
a. Atisara [Cha. Sa. Chikitsa Sthana 19, Su. Sa. Uttara Tantra. 40 ]
b. Grahani [Cha. Sa. Chikitsa Sthana.15, Su. Sa.Uttara Tantra 40, A. Hr. Nidana Sthana 8]
c. Pravahika [Cha.Sa. Chikitsa Sthana 19]
d. Pakvashayagata vata [Cha. Sa. Chikitsa Sthana 28 /28-29]
Among these conditions, symptoms of vata predominant grahani show more resemblance with IBS. Poor digestion, hyperacidity, roughness in the body and flatulence during and after digestion are observed in this condition. The patient frequently passes stool with difficulty. The consistency of faecal matter is liquid mixed with hard stool, associated with sound and frothiness. [Cha. Sa. Chikitsa Sthana15/6-10]
In pravahika, there is frequent expulsion of stool containing mucus in less quantity accompanied by pain and straining (tenesmus).
Dietary modifications including more dietary fibers, psycho-social therapies, drugs like anticholinergics, antidepressants, antidiarrheals, anxiolytics and those acting on serotonin receptors are being used in the management of IBS. Probiotics have a greater role to enhance or support the bacterial flora in the gut.
Principles of treatment of IBS
The treatment principles of vataja grahani, atisara and pakwashayagata vata are used in the management of IBS. The psychological health component is taken care of by therapies like the pouring of liquid medicines like oil, medicated butter milk etc on the forehead (shirodhara/ takradhara) and anointment of medicated paste on scalp(shirolepa).
Sitz bath with lukewarm medicated water(avagaha sweda), enema using medicated oil or ghee(anuvasana basti) are effective procedures in this condition.
The treatment principles can be divided into two as per the stages or phases:
a)In Diarrhoea dominant stage, drugs having the properties of enhancing digestive power (agni dipana), styptic (grahi), and improving the strength of tissues (dhatubalakara) are used.
b)In Constipation dominant stage, drugs that produce the effects of clearing the minute channels (srotoshodhana), enhancing the digestive power (koshthagnidipana), and promoting the downward movement of vata (vatanulomana) are used.
In the first phase of IBS, mainly medicines in the powder (churna) form or medicated liquids (paneeya kalpana) are used to promote digestive power. In diarrhoea dominant stage, “panchakola churna” and in constipation dominant stage, “ vaishwanara churna” are the drugs of choice.
In the second phase, if the person acquires good digestive capacity(agni dipti),medicated ghee (ghritas) and linctus preparation (avaleha) are used.These medicines pacify vata(vatahara) and help to maintain the proper function of digestive fire(agnisatmyakara). For example, dadimadi ghrita or sukumara ghrita mixed with rock salt(saindhava) can be prescribed.
The formulations like brihat gangadhara churna, dadimadi churna, hingvashtaka churna, jatilavangadi churna, kapitthashtakam churnam, chitrakadi vati, changeryadi gutika, manasa mitra vatakam, parushakadi lehya, kutajadi lehya, panchamrita parpati, kshara parpati, swarna parpati, with butter milk and medicated meat soups are also effective in this condition.
The dietary items like wheat, maize, barley, peas, black gram, soya bean, kidney bean, potato, sweet potato, onion, ground nut, chilly, oily food, chicken, red meat, crabs, mango, pineapple, apple, watermelon, cashew, fig, pumpkin papaya and jackfruit shall be avoided by the patients of IBS.
The diet plan including the use of old rice, gourd, coriander leaves, lentil, green grams soup, black pepper, dried ginger, pomegranate, nutmeg buttermilk, and hot water are suitable.
In a clinical study on IBS, by Raksha Mer & H. M. Chandola (2004), the effect of kutajadi avaleha alone and kutajadi avaleha along with medhyarasayana ghrita was compared. Better results were observed in the combined group. This shows the importance of addressing the psychological component in the treatment protocol.
Buttermilk has an astringent taste (kashaya rasa) and hot potency (ushna virya). It increases the digestive power (deepana) and absorbs fluid from the stool (grahi). It decreases aggravated kapha and rectifies the digestive process. It’s sweet and sour taste do not provoke vata. Its property of “madhura vipaka”, does not cause the aggravation of pitta. So, it is best to keep the balance of all the three dosha in gut.
Buttermilk contains all essential macronutrients. It has a cooling effect on the digestive tract. It encourages digestion and treats gut ailments. It is effective against dehydration. It provides calcium without fat and is rich in vitamins, like riboflavin.
Rejuvenating (rasayana) drugs for gut health
Emblica officinalis (amalaki), Eclipta alba (bhringaraja) and Asparagus racemosus (shatavari) are recommended for the health of stomach.
Aegle marmelos (bilva), Holarrhena antidysenterica (kutaja) and Terminalia chebula (haritaki) are the best rasayana herbs for the health of intestine.
Summary and Conclusion
- Ayurvedic diagnosis of Acid Peptic disorders mainly depends on etiological factors, clinical manifestation of disease (symptomatology), relieving factors (upashaya) and aggravating factors (anupashaya).
- Ayurvedic management depends on the assessment of dominant symptoms, assessment of involved dosha (dysregulation of kledaka kapha, pachaka pitta and samana vayu) and its dominant properties (amshansha Kalpana), status of agni and ama.
- Drugs that correct ama, optimize agni, regulate samana vayu, pacify aggravated pachaka pitta, protect kledaka kapha, aid digestion, promote smooth transit of food in the gut, integrate intestinal motility are most suitable to treat acid peptic disorders in Ayurveda.
- The principle of treatment includes that of Amlapitta, Annadrava shula, Parinama shula, Atisara & Grahani.
- Modifications of diet, life style and stress management have greater role in their management.
- Integration of tradition and technology is the need of hour.
In present scenario, ancient knowledge shall be enriched with recent updated diagnostic tools to achieve the goal of a healthy and happy life.
Interaction Session
Q: How to treat H.pylori infection through Ayurveda?
A. There is no specific Ayurvedic drug proven for its action on eradicating H.Pylori through any research works. We need to adopt the principles of the treatment of krimi. Many single drugs like Holarrhena antidysenterica (kutaja), Butea monosperma (palasha), Embelia ribes (vidanga) etc. and formulations like krimimugdar rasa, krimikuthara rasa etc. have “krimighna” properties. If we make some combinations of these and try, it can have good results along with the amlapitta chikitsa.
Q: Usually in acid-peptic diseases, asava- arista preparations are not prescribed. But in the management of ulcerative colitis you have mentioned some asava- arishta preparations. Can you elaborate on the concept a little further?
A. There are a lot of differences in preparation of asava -arishta in traditional method of fermentation and the one which is followed in the current era. The readymade preparations available nowadays can cause undesirable effects especially in the condition of acid peptic disorders. But if they are prepared in the traditional method, and used judiciously, it can give good results.
Link to video lecture: https://fb.watch/8l8TUYT2eZ/